If your dentist informs you that you’ve got periodontal disease, you’ll need to work together to create a treatment plan that improves your gum health. Periodontal disease can affect anyone, with roughly half a million Americans over 30 suffering from gum disease. Fortunately, it’s treatable with minimally invasive methods by your dentist if caught early.
What is Periodontal Disease?
Periodontitis, the medical term for periodontal or gum disease, is an infection affecting both the gums and bones that support your teeth.
A buildup of bacteria on your teeth leads to gingivitis, the early stage of periodontal disease. The initial condition may lead to a full-blown case of periodontitis if left untreated. Advanced periodontitis can damage teeth and compromise your overall oral health.
Treatment methods for periodontal disease vary depending on the severity of the case and your dentist’s advice.
Non-Surgical Treatments for Periodontal Disease
Modern dental technology and procedures can detect gum disease early, allowing your dentist to manage it before it becomes severe.
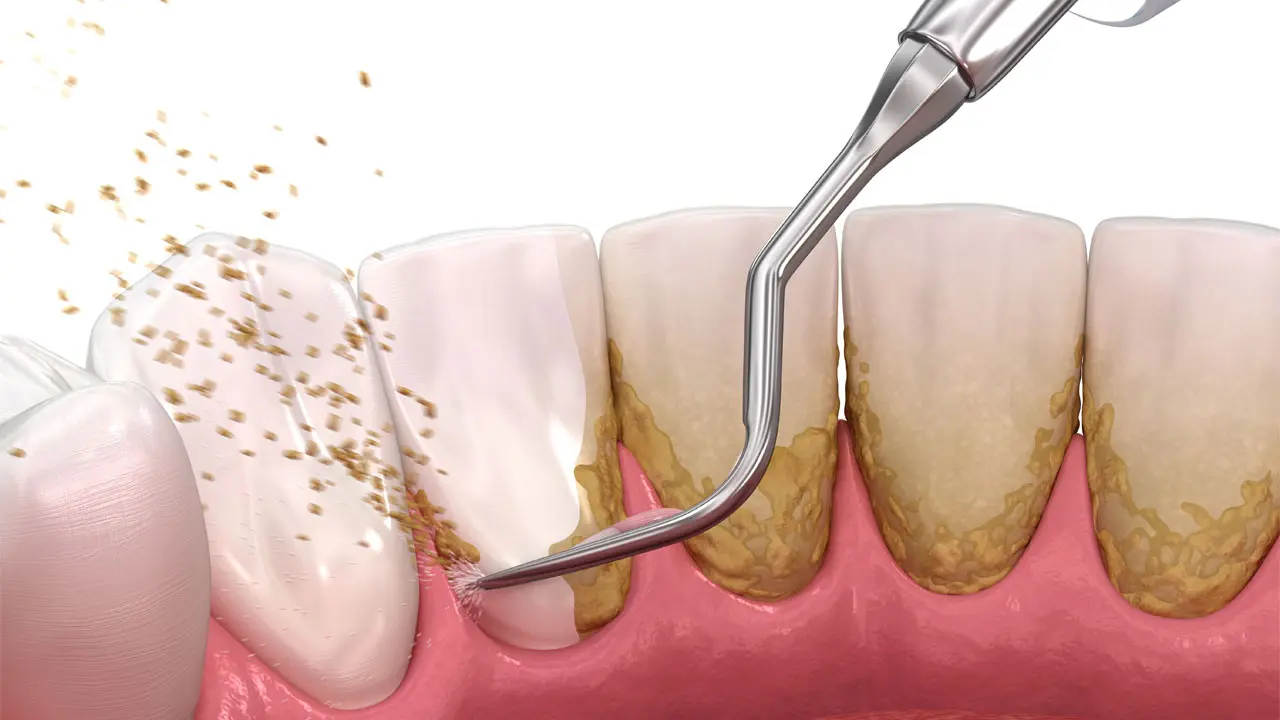
- Professional Dental Cleanings. When you go for general dental routine visits, the dentist removes plaque and tartar on the teeth and along the gum line. Your dentist may recommend more frequent cleanings if gum disease is still in its early stages.
- Planing and Scaling. You may need a deep cleaning both above and below the gum line from your dentist. Following the application of a topical anesthetic, plaque and tartar are scraped off the teeth (scaling) and smoothed over to prevent bacterial buildup (planing).
Surgical Treatments for Periodontal Disease
In advanced cases, surgery may be necessary to repair the damage caused by periodontitis. It is best to consult your dentist or periodontist regarding how to proceed, but you may be required to undergo one of the following procedures:
- Flap Surgery (pocket reduction surgery). A periodontist makes thin, microscopic incisions in your gums to expose the roots and perform scaling and root planing with greater precision. Due to the bone loss caused by periodontitis, the gum will need to be stitched back into place after the bone has been recontoured. Once your gums heal, dental cleanings will be much easier.
- Soft Tissue Grafts. Losing gum tissue causes your gum line to recede. The soft tissues, in some cases, need to be strengthened by removing some tissue from the roof of your mouth (palate) or by planting tissue from another donor source near the damaged area.
- Guided Tissue Regeneration. This allows the germ-damaged bone to regenerate. The periodontist places biocompatible tissue between your bone and your tooth to keep unwanted tissues out of the area that is healing.
- Dental Implants. You can also use dental implants to replace teeth if you have lost them to gum disease. These are titanium posts inserted into the jawbone. After the implants have bonded to the jawbone, the dentist adds an abutment and installs a customized prosthetic tooth. A dental implant is a permanent solution for missing teeth, unlike dentures and bridges, which may require replacements regularly.
Follow-Up Care After Treatment
The best way to avoid periodontitis is to maintain your dental health after gum disease treatment. Every few months, you may need to visit your dentist for deeper cleanings. These cleanings ensure that bacteria levels on the teeth and gum line remain under control, preventing further damage.
You may also be advised to keep up your regular oral hygiene, including brushing your teeth twice a day and flossing once daily.
Early Intervention is Crucial
Periodontal disease needs to be treated early, just as any major illness. It’s best to get gum disease under control as soon as you notice the signs, so you don’t have to worry about long-term complications. Call our practice to arrange a hygiene cleaning and dental exam if you have any concerns about the possibility of gum disease.